Introduction
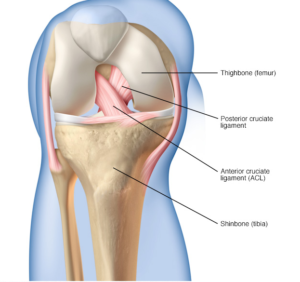
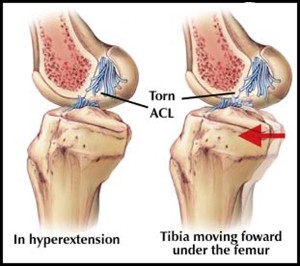
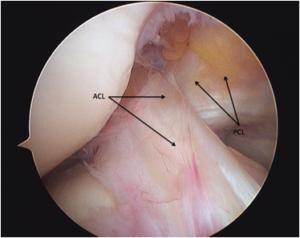
The anterior cruciate ligament (ACL) is a 3-4cm long band of fibrous tissue that connects the femur (thigh bone) to the tibia (shin bone). It helps stabilise the knee joint when performing twisting actions. The cruciate ligament is usually not required for normal daily living activities, however, it is essential in controlling the rotation forces developed during side stepping, pivoting and landing from a jump.
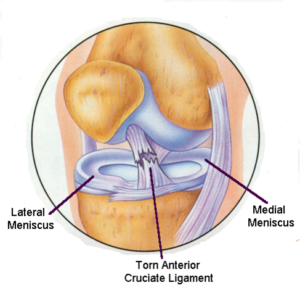
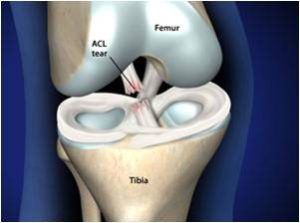
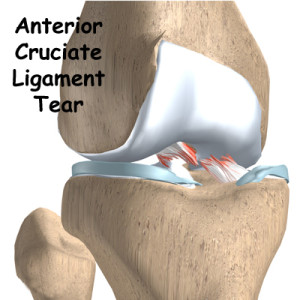
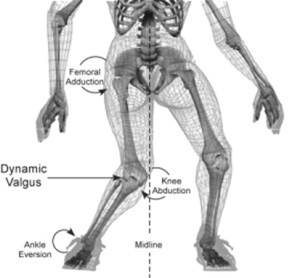
It has to withstand tremendous forces during activity and is very vulnerable. Under circumstances, usually sport, the stress is more than the ligament can stand and it ruptures. Typical mechanisms of injury are a severe blow to the outside or inside of the knee causing a severe force, turning, twisting, jumping, sharp acceleration and deceleration, change of direction at speed and walking, jogging or running on uneven or unpredictable surfaces. When this happens the knee is usually acutely painful and a “pop” or “crack” may be felt or heard by the patient. The knee becomes swollen, usually within a few hours. Following this the knee may settle down but because the ruptured ligament rarely heals satisfactorily, the joint will feel vulnerable and is likely to give way if stressed. Pain, swelling and stiffness may also occur. These problems is predominately seen in young, active, sporting individuals but can occur at any age and may be caused by any type of accident e.g. domestic injury or road traffic accident.
Initial treatment of any knee ligament injury should consist of ice packs, compression bandages and crutches. It is difficult to weight bear for several days, however, after seven to ten days the swelling settles and walking is possible with the joint gradually returning to full movement.
Further episodes of instability result in multiple injuries to the cartilages and the joint surfaces. Damage to these structures eventually leads to osteoarthritis.
WHY DOES THE ANTERIOR CRUCIATE LIGAMENT FAIL TO HEAL?
Unlike other ligaments about the joint, the ACL passes through the joint and is surrounded by joint fluid. Other ligaments heal by scar formation, however due to the unique location of the ACL the bleeding is uncontained, filling the joint, causing pain and swelling. The blood irritates the knee joint’s lining to produce synovial fluid. This fluid is designed to dissolve and prevent blood clotting within the joint. Without blood clot, scar tissue does not form. The result is that the ACL rarely heals in continuity.
RATIONALE FOR TREATMENT
The goal of treatment of an injured knee is to return the patient to their desired level of activity without risk of further injury to the joint. Each patient’s functional requirements are different.
Treatment may be without surgery (conservative treatment) or with surgery (surgical treatment). Those patients who have a ruptured ACL and are content with activities that require little in the way of side stepping (running in straight lines, cycling and swimming) may opt for conservative treatment.
Those patients who wish to pursue competitive ball sports, or who are involved in an occupation that demands a stable knee are at risk of repeated injury resulting in tears to the menisci, damage to the articular surface leading to degenerative arthritis and further disability. In these patients, surgical reconstruction is recommended.
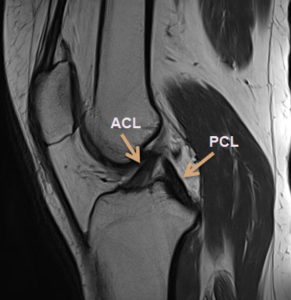
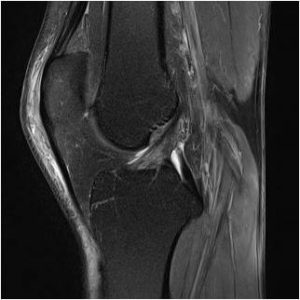
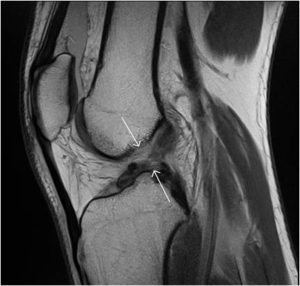
Diagnosis
MRI scan
TREATMENT OPTIONS
Conservative Treatment
Conservative treatment is by physical therapy aimed
at reducing swelling, restoring the range of motion of the knee joint and restoring full muscle power.
Proprioceptive training to develop the necessary protective reflexes are required to protect the joint for normal daily living activities.
As the cruciate ligament controls the joint during changes of direction, it is important to alter your sports to the ones involving straight line activity only. Social (non-competitive) sport may still be possible without instability as long as one does not change direction suddenly.
Surgical Treatment
Patients who are unable (generally young adults) or those unwilling to lower their level of activity, are at risk of causing further damage to their knee should they return to sporting activity and are advised to undergo surgical reconstruction.
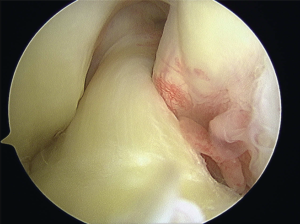
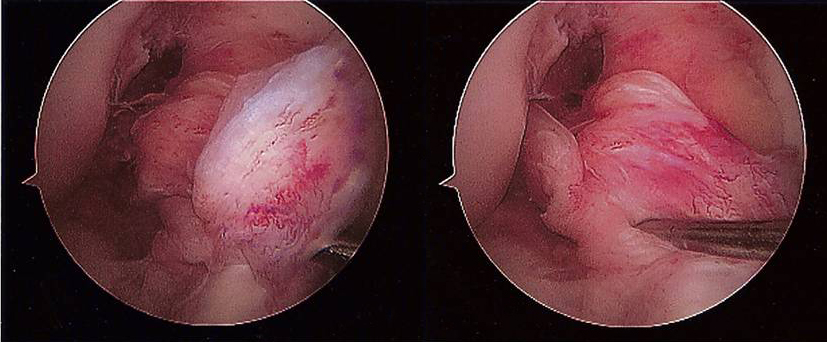
Reconstruction involves placing a graft inside the knee by arthroscopic surgery (keyhole). A
>90% success rate is normal with some deterioration over time depending upon other damage within the joint.
Although ACL reconstruction surgery has a high probability of returning the knee joint to near normal stability and function, the end result for the patient depends largely upon a satisfactory
rehabilitation and the presence of other damage within the joint.
Advice will be given regarding the return to sport- ing activity, dependant on the amount of joint dam- age found at the time of reconstructive surgery.
It is important to preserve damaged joint surfaces by restricting impact loading activity to delay the onset of degenerative osteoarthritis later in life.
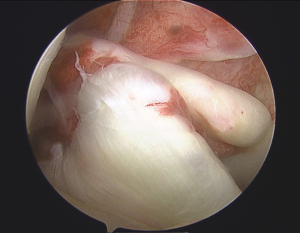
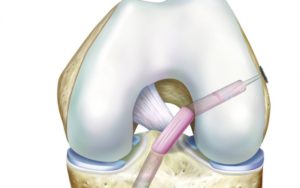
In the surgery a graft will be harvested to use to reconstruct the torn ligament. Usually two of the hamstring tendons are taken, but sometimes other suitable graft choices are used. This will be discussed with you prior to the operation. The remnants of the torn ACL are removed with keyhole surgery and tunnels are made in the tibia (shin bone) and femur (thigh bone) to allow the graft to be positioned across the knee. The new reconstructed ligament is then fixed at both ends to secure it in place.
Anatomical ACL reconstruction
Anatomic placement of an anterior cruciate ligament (ACL) graft is critical
to the success and clinical outcome of ACL reconstruction. Anatomic ACL graft placement is defined as positioning the ACL femoral and tibial bone tunnels at the center of the native ACL femoral and tibial attachment sites.
Clinical studies have demonstrated that non-anatomic ACL graft placement is the most common technical error leading to recurrent instability following ACL reconstruction.
[ ACL reconstruction has been commonly performed using a transtibial technique in which the ACL femoral tunnel is drilled through a tibial tunnel positioned in the posterior half of the native ACL tibial attachment site. In the transtibial technique, positioning the ACL tibial tunnel in the posterior half of the ACL tibial attachment site is dictated by the need for the endoscopic drill bit to reach the region of the ACL femoral attachment site and the desire for the ACL graft to avoid impingement against the roof of the intercondylar notch when the knee is in full extension. However, the resulting ACL femoral tunnel is often positioned too high and too deep in the intercondylar notch, away from the native ACL femoral attachment site.
An ACL graft positioned at a posterior tibial and a high-deep femoral attachment site will be vertically oriented in both the coronal and sagittal planes. Biomechanical studies have shown that a vertically oriented ACL graft may resist the motion of anterior tibial translation, but may fail to control the combined motions of anterior tibial translation and internal rotation which occur during the pivot-shift phenomenon.3 The inability of a vertically oriented ACL graft to control these combined motions may result in the patient experiencing continued symptoms of instability and giving-way episodes due to the pivot-shift phenomenon.]
In the Anatomical ACL reconstruction technique, which is used in most advanced centres of the world, we use an accessory anteromedial portal with the knee flexed to 120 degrees.
This approach provides several advantages compared to the traditional transtibial technique:
- The ACL femoral tunnel is drilled independently of the tibial tunnel, which results in consistent placement of the femoral tunnel within the native ACL femoral attachment site.
- The angle of the ACL tibial tunnel does not have to be compromised to accommodate drilling of the ACL femoral tunnel. Therefore, the surgeon can opt to drill a steeper and thus longer tibial tunnel. A longer tibial tunnel minimizes the potential for graft-tunnel length mismatch and allows longer bone-tendon- bone graft constructs to be utilized.
- Although guides are available, the medial portal technique does not require any special guides or instrumentation.
- Inserting an ACL femoral interference fixation screw through the same medial portal which was used to drill the ACL femoral tunnel minimizes screw-tunnel divergence.
- The medial portal technique provides improved arthroscopic visualization during drilling of the ACL femoral tunnel since the femoral tunnel can be drilled under ideal arthroscopic conditions, without the loss of joint distention due to fluid extravasation out of the tibial tunnel.
Graft options
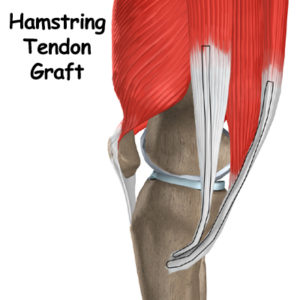
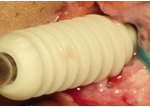
Hamstring graft, Bone- patellar tendon- Bone, Allograft or synthetic grafts are the options available for ACL reconstruction. Hamstring is the preferred graft as there is minimum donor site morbidity and the remaining hamstring strengthen over time to cover-up for the transferred hamstrings.
Patellar tendon graft will leave a long scar in the front of the knee and many patients have pain on the front of the knee after that. Hamstring graft can be harvested through the same incision we use to drill the tunnel for graft insertion. Allograft and synthetic grafts have unacceptably high failure rates and are used only in rare situations when no autograft is available.
Fixation methods
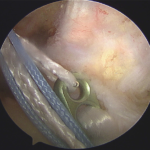
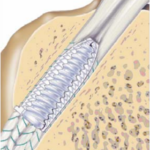
Femoral fixation – Superior fixation of the graft in the femoral tunnel is done with an all-inside technique using Endobutton (smith-nephew usa).
What happens before and after surgery?
Before surgery
Before surgery your knee must have a nearly normal comfortable range of movement. For the weeks lead- ing up to the surgery you should start some exercises that will help with your recovery. These are explained in more detail in the prehabilitation/ rehabilitation section.
Healthy patients are admitted on the night before their surgery. You should inform your surgeon and anaesthetist, of any medical conditions or previous medical treatment as this may affect your
operation.
It is extremely important that there are no cuts, scratches or pimples on your lower limb as this greatly increases the risk of infection. Your surgery will be postponed until the skin lesions have healed. You should not shave or wax your legs for one week prior to surgery.
Patients should cease smoking and taking the oral contraceptive pill 6 weeks prior to surgery as this increases the risk of thromboembolism (life threatening blood clots).
After the operation you will normally be required to stay in hospital for one or two nights.
COMPLICATIONS
General complications related to surgery
Deep vein thrombosis and pulmonary embolus: Although this complication is rare following arthroscopic surgery, a combination of knee injury, prolonged transport and immobilisation of the limb, smoking and the oral contraceptive pill or hormonal replacement therapy all multiply to increase the risk. Any past history of thrombosis should be brought to the attention of the surgeon prior to your operation. The oral contraceptive pill, hormonal replacement therapy and smoking should cease 6 weeks prior to surgery.
Pneumonia: Patients with a viral respiratory tract infection (common cold or flu) should inform the surgeon as soon as possible and will have their sur- gery postponed until their chest is clear. Patients with a history of asthma should bring their inhalers to hospital.
Complications specifically related to your knee reconstruction surgery.
Infection is a serious but rare complication. Surgery is carried out under strict germ free conditions in an operating theatre. Antibiotics are administered intravenously at the time of your surgery.
Any allergy to known antibiotics should be brought to the attention of your surgeon or anaesthetist.
Despite these measures, following arthroscopic ACL reconstructive surgery there is about a 0.5% chance of developing an infection within the joint. This may require treatment with antibiotics or may require hospitalisation and arthroscopic wash-out of the joint. Subsequent to such procedures prolonged periods of antibiotics are required and the post operative recovery is slowed.
Postoperative bleeding and marrow exuding from the bony tunnel may track down the shin causing red inflamed painful areas. Characteristically when standing up the blood rushes to the inflamed area causing throbbing this should ease with elevation and ice packs. This may end with a bruise and slight swelling around the ankle usually lasting about one week. This is a normal postoperative reaction and only delays short term recovery. Excessive bleeding resulting in a haematoma is known to occur with patients taking aspirin or on steroidal anti- inflammatory drugs. They should be stopped at least one week prior to surgery and probably should not be taken all all.
Nerve injury. Due to the skin incision, patients may notice a numb patch on the outer aspect of their leg past the skin incision. This is of no functional significance and is unavoidable. The numb patch tends to shrink with the passage of time and does not affect the result of the reconstructed ligament.
Graft failure due to poorly understood biologic reasons occurs in approximately 1% of grafts and a further 1% of grafts rupture during the rehabilitation programme. After two years if you return to normal activities the risk of further ACL injury returns to near normal (about 1% each year for patients returning to high intensity sports), the risk of rupturing the reconstruction is similar to that of rupturing the ACL in the other knee.
Pain and stiffness. Rarely patients develop pain and stiffness in the knee after ACL reconstruction. This can normally be resolved with intensive physiotherapy. Occasionally further surgery may be required.
AFTER THE OPERATION
You will wake up in recovery with the knee bandaged. You may have a small drain coming from the knee to help drain any excess bleeding and reduce the swelling. You will be given pain medications if required. It is safe to move the knee, but you will be encouraged when resting to keep the knee straight.
It is safe to fully weight bear through the knee straight away, but often it is more comfortable to start walking with some elbow crutches. Most patients will only use these for the first few days.
By two to three weeks you should be walking normally. It is normally safe to drive when you are walking normally and putting all your weight through the leg.
The knee will have a tendency to swell in the first six weeks. It is important to ice the knee between exercises and when resting to keep it elevated.
You will be given some exercises to help rehabilitate the knee. The rehabilitation is split into three phases
Physiotherapy
Physiotherapy is commenced immediately post-operatively and should continue for 4-6 weeks. By 14-21 days following surgery you should be able to walk without crutches. Sedentary and office workers may return to work approximately 5-7 days following surgery. Most patients should be walking normally 21 days following surgery although there is considerable patient to patient variation.
Driving a car – Should the left knee be involved then driving an automatic car is possible as soon as pain allows. You must not drive a motor vehicle whilst taking severe pain killing medications. Should the right knee be involved driving is permitted when you are able to walk without crutches. It would be comfortable to start driving in 4-6 weeks after surgery.
Rehabilitation exercises should be continued intensively until 4 to 6 weeks when jogging under controlled conditions is commenced.
Sports – Playing sport non-competitively or training is possible at 4 to 6 months. Training may commence when an adequate rehabilitation of the thigh musculature has occurred. A return to competitive sport is permitted at 9-12 months following surgery, again provided that there has been a complete rehabilitation and the joint is demonstrated to be stable.

 Call us:+91-484 2885910 (Reception Orthopedics; 9am to 5pm Mon-Sat), +91-484-2885621 (22,23,24)
Doctor's mobile - +91 9497559755 (whatsApp anytime)
Call us:+91-484 2885910 (Reception Orthopedics; 9am to 5pm Mon-Sat), +91-484-2885621 (22,23,24)
Doctor's mobile - +91 9497559755 (whatsApp anytime)