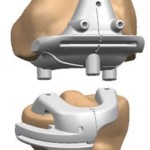
Who Needs Knee Replacement Surgery?
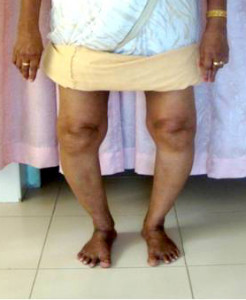
Knee replacement surgery is considered if you have a stiff, painful knee that makes it difficult to perform even the simplest of activities, and other treatments are no longer working. This surgery is generally reserved for people over age 50 who have severe osteoarthritis.
This is done for any type of degeneration of the knee which may be due to osteoarthritis, inflammatory conditions such as rheumatoid arthritis and also for post traumatic arthritis.
As the life expectancy of our population is increasing the degenerative problems to the joints are also on the rise. Most cases of osteoarthritis can be treated with medications, physical therapy and activity modifications.
Degenerative Joint diseases or osteoarthritis is a progressive problem. There are measures to slow or stall the progression, but you cannot reverse it. It is like your age, it only goes forwards. When the degenertion has progressed beyond a certain level, we have to consider surgical replacement of the cartilage lining with metallic (Cobalt-chrome or Titanium) lining , which is a joint replacement surgery.
-

- Difference between cartilage lining in normal and osteoarthritic knee
-
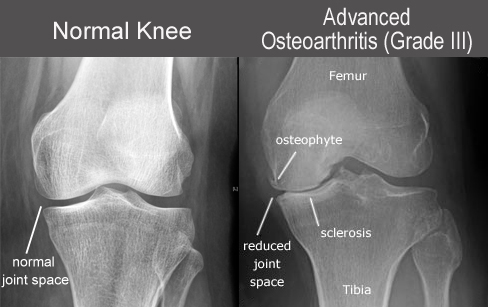
- When arthritis progresses, the bones rub against each other and cause pain and instability. The xray on the left side shows normal joint gap and that on the right shows reduced joint gap due to osteoarthritis
A highly specialized liner made of polyethylene is inserted between the two metallic surfaces to replace the worn meniscus. There are broadly two types of knee replacements- unicompartmental (partial) and total knee replacement.
WHAT IS MINI-INVASIVE KNEE REPLACEMENT ?
Smaller incision, less pain, faster mobility, high flexion – Know more>>
What Happens During Knee Replacement Surgery?
Once you are under spinal/epidural anesthesia (numb below the waist) or general anesthesia (meaning you are temporarily put to sleep), an 6- to 10-inch cut is made in the front of the knee. The damaged part of the joint is removed from the surface of the bones, and the surfaces are then shaped to hold a metal or plastic artificial joint. The artificial joint is attached to the thigh bone, shin and knee cap either with cement or a special material. When fit together, the attached artificial parts form the joint, relying on the surrounding muscles and ligaments for support and function.
What are the most important technical aspects for a knee replacement?
- Correct surgical technique – Good surgical technique can allow you to have a near-normal joint that lasts for many years (15 to 20 years, or more). With less disruption of your tissues there will be lesser pain and you return to normal activity earlier. Incorrect surgical methods can lead to postoperative problems like mal-alignment, instability and infection which are very difficult to treat.
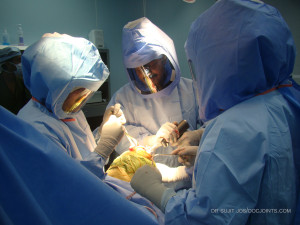
- Strict Sterile precautions – A very clean theatre dedicated to joint replacements is very important to prevent a postoperative infection. If a joint replacement surgery is done well the recovery and wound healing are very fast.
At PVS memorial Hospital theatre, we use –
-
- A modular imported Operation theatre – of Johnson and Johnson dedicated to ultrasterile joint replacement surgeries.
- Hepa filters – Filters out particles as small as 3000th of a millimeter.
- double laminar air-flow – Horizontal and Vertical
- Body suits with helmets – to prevent unsterile particles falling into the wound like bone bits, cement, or irrigating fluid which may be touch the surgeon’s or assistant’s head or face and fall back into the wound without our knowledge during the surgery.
- Special water filters for hand wash fluid before surgery
- 100% disposable drapes – imported
- All this at a minimal cost difference compared to centres where the doctors operate in an ordinary operation theatre
We strive to provide the best quality procedure to you which makes us the best and trustworthy centre for a joint replacement surgery.
What Are Recent Advances in Knee Replacement Surgery?
MINIMALLY INVASIVE SUBVASTUS APPROACH TO A TOTAL KNEE REPLACEMENT
Minimally invasive surgery has revolutionized knee replacement surgery as well as many fields of medicine. Its key characteristic is that it uses specialized techniques and instruments to enable the surgeon to perform major surgery without a large incision.
Minimally invasive knee joint replacement called the SUBVASTUS APPROACH requires a much smaller incision, 3 to 5 inches, versus the standard approach and incision. The smaller, less invasive approaches result in less tissue damage by allowing the surgeon to work between the fibers of the quadriceps muscles instead of requiring an incision through the tendon. It may lead to less pain, decreased recovery time and better motion due to less scar tissue formation.
Currently this less invasive procedure is performed by only a small percentage of orthopedic surgeons in North America. Researchers continue looking at the short-term and long-term benefits of minimally invasive versus traditional knee replacement surgery. Read More>>

Minimally Invasive Subvastus Incision without violating the vastus medals muscle
Unicondylar Knee Replacement
This is a less invasive alternative to Total Knee Replacement. This procedure is commonly performed on younger, more active patients. The cost is minimally lesser than a total knee replacement, but the main advantage is that the Knee feels very much natural. The incision is much smaller, pain is much less and recover is much faster. Read more>>
Gender Specific Knee – Special knee for Women
Recent direct to consumer marketing regarding gender specific, or women’s knee replacements has seemingly brought this subject to light. Traditional knee joint implants were originally designed as average sizes for the general population with universal femoral (thigh bone) parts that were not even specific for the right or left side.
Women’s knees are generally smaller than men’s and require narrower profiles that have been incorporated into these new designs. However, the prospective knee replacement patient needs to discuss these specific issues with their surgeon, so as to create the best preoperative plan for a successful knee replacement.

Gender Specific Knee designs give an active life after a knee replacement for women
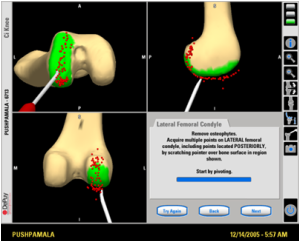
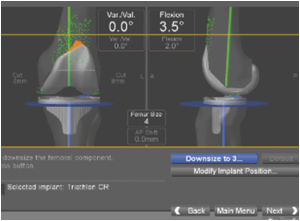
Computer Navigation
Assistance of Computer Navigation increases the accuracy of Implant placement during a Knee Replacement. Restoring normal mechanical axis of the limb in the coronal plane has always been one of the main goals for knee arthroplasty surgeons in order to reduce the risk of early implant failure as a result of accelerated wear and aseptic loosening.
PATIENT SPECIFIC INSTRUMENTATION (PSI)
PSI uses a patient’s MRI and x-rays to create custom surgical instrumentation. Nylon blocks are sintered to make custom cutting blocks. Personalized blocks are used for preparing the bones for implantation. In addition to increasing the accuracy of the cuts and limb alignment, it negates the need for intramedullary drilling and thus reduces the risks for fat embolism and also reduces blood loss. This has superseded computer navigation as it saves valuable operating time thereby reducing infection risk and anesthesia time which were more for a conventionally navigated knee.
What Happens After Knee Replacement Surgery?
The average hospital stay after knee joint replacement is usually three to five days. The vast majority of people who undergo knee joint replacement surgery have dramatic improvement. This improvement is most notable one month or more after surgery. The pain caused by the damaged joint is relieved when the new gliding surface is constructed during surgery.
After knee joint replacement, people are standing and moving the joint the day after surgery. At first, you may walk with the help of parallel bars, and then a walking device — such as crutches, walker, or cane — will be used until your knee is able to support your full body weight. After about six weeks, most people are walking comfortably with minimal assistance. Once muscle strength is restored with physical therapy, people who have had knee joint replacement surgery can enjoy most activities (except running and jumping).
When can you return to normal activity after Knee Replacement surgery?
You can stand up the very next day after the surgery with the newer methods we adopt during the surgery and other pain control measures. You will be using a walking aid which will be needed for 4 to 7days, depending on the previous muscle power and general health.
The staples on the knee can be removed in 10 to 14 days time. The knee can be washed normally during bath after a couple more days.
There will be exercises for the knee during the first month which you can do by yourself or a physiotherapist can help you twice or thrice a week. In a months time most of the patients are ready to go out of the house for small functions.
In 3 months time the healing of the internal tissues will be complete and the knee will start feeling almost like it was before the osteoarthritis started.
You can start climbing stairs by about 3 weeks after the surgery. But many patients do that much earlier like Mrs Fatma Khalfan who was climbing 2 floors by 10days. That is the benefit of the newer muscle sparing approach that we use for surgery.
Watch the patient education program on World Arthritis day 2016 at PVS Memorial Hospital, Kochi.
There were talks on arthritis, preventive and corrective measures. Renowned writer Prof MK Sanu, Movie director Mr Babu Narayanan and Writer Mrs Ambika Nayyar presided over the function.
There was even a thiruvathira dance performance by Knee replacement patients. They wanted to show the world their regained functional ability and quality of life after joint replacement.
At PVS memorial Hospital we now have more options than ever before to “custom fit” each prosthesis to each patient. We utilize the latest surgical approaches, state-of-the-art implant designs and post-operative protocols to optimize each patient’s return to function. Ultimately, it is the skill of the surgeon, the fit of the prosthesis, the physical therapy and nursing protocols and the patient’s hard work that make a successful knee replacement surgery. The Knee replacement team headed by Dr Sujit Jos does the highly successful Mini-Invasive Subvastus Knee Replacement that is less painful and allows you to regain normal activity faster than Regular medial parapatellar approach for Knee replacement surgery which is still practised in most of the centres. Read more>>
Know about Unicondylar knee replacement for isolated unicompartmental arthritis. This gives more functional ability and prevents progression of arthritis in relatively younger patients
Watch television talks on Osteoarthritis by dr sujit jos>>
https://www.youtube.com/watch?v=q0Yq92cq20A

 Call us:+91-484 2885910 (Reception Orthopedics; 9am to 5pm Mon-Sat), +91-484-2885621 (22,23,24)
Doctor's mobile - +91 9497559755 (whatsApp anytime)
Call us:+91-484 2885910 (Reception Orthopedics; 9am to 5pm Mon-Sat), +91-484-2885621 (22,23,24)
Doctor's mobile - +91 9497559755 (whatsApp anytime)