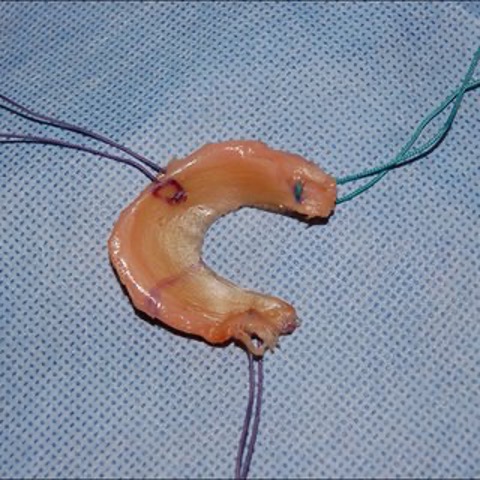
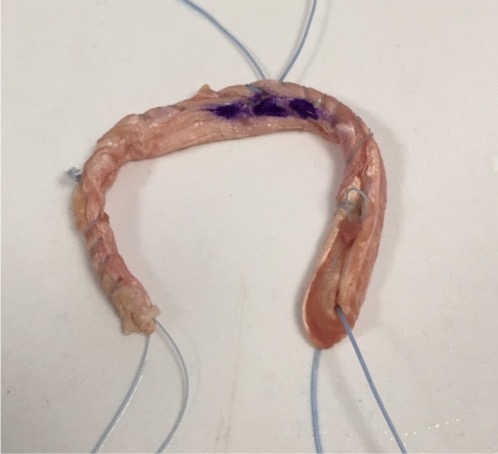
To know basics about Meniscus transplantation

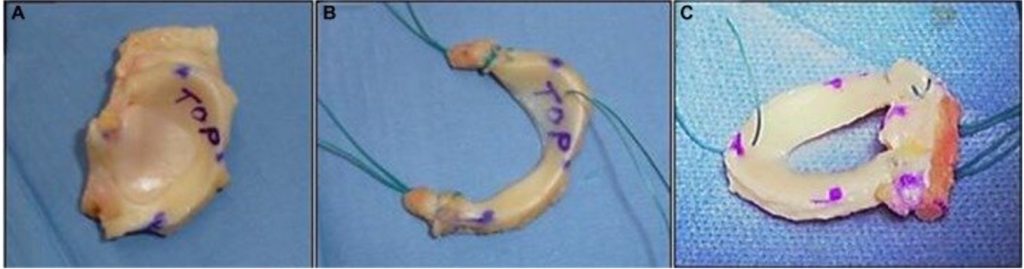
1. Concept & Tissue Source
| Feature | Meniscal Allograft Transplant (MAT) | Tendon Autograft (ST / PL “Neomeniscus”) |
|---|---|---|
| Tissue source | Size-matched cadaveric meniscus (fresh-frozen/cryopreserved). | Patient’s own semitendinosus or peroneus longus tendon, shaped into a meniscus-like construct. PMC+2PubMed+2 |
| Biological nature | Native fibrocartilage with meniscal collagen architecture. | Tendon (collagen I) that remodels towards fibrocartilaginous tissue over time (“neomeniscus”). PMC+1 |
| History | >30 years of clinical use, multiple mid–long-term series. ScienceDirect+2Orthopedic Reviews+2 | Emerging; mostly biomechanical work, pilot series, case reports, and early comparative data. Jassm+4PMC+4 |
2. Indications & Patient Selection
Meniscal Allograft
- Symptomatic meniscal deficiency after subtotal/total meniscectomy.
- Young / middle-aged, stable, well-aligned knees with no or mild chondral damage. Orthopedic Reviews+1
- Often combined with ACL reconstruction, HTO, or cartilage procedures in “biologic knee preservation” packages. Orthopedic Reviews
Tendon Autograft (ST / PL)
- Same basic indications: symptomatic post-meniscectomy knee in young patients.
- Particularly attractive where allograft is:
- Unavailable / legally restricted / prohibitively expensive. PMC+2PubMed+2
- Some techniques used for segmental reconstruction rather than whole-meniscus replacement. PubMed+1
Contraindications (advanced OA, malalignment not corrected, unaddressed instability) are broadly similar for both.
3. Surgical Technique & Sizing
| Aspect | Allograft | ST / PL Autograft |
|---|---|---|
| Sizing | Relies on radiographic/MRI templating and exact meniscal dimensions; size mismatch is a known problem. ScienceDirect+1 | Graft diameter and length can be adjusted intra-op; some authors emphasise less dependence on exact pre-op sizing. PubMed+2ISAKOS+2 |
| Fixation | Bone plugs / bone bridge or soft tissue fixation; root reattachment + peripheral sutures. Orthopedic Reviews+1 | Tendon looped or doubled, sometimes combined with collagen membrane or fibrin clot; roots recreated via tunnels and peripheral suturing to capsule. PMC+2PMC+2 |
| Technical familiarity | Well-standardised in high-volume centres. | Techniques are heterogeneous; still evolving, no universal standard. Lippincott Journals+1 |
4. Biomechanics
Allograft
- Multiple cadaveric studies show MAT can restore contact area and reduce peak contact pressures close to native meniscus, though extrusion and subtle kinematic changes remain issues. ScienceDirect+1
Semitendinosus / Peroneus Longus Autograft
- Doubled semitendinosus autograft lateral “meniscus” significantly improved tibio-femoral contact mechanics and kinematics compared with meniscectomy, approaching native values. PMC
- Preclinical and early human data suggest tendon autografts can remodel and function as a load-sharing structure, but long-term chondroprotection is still unproven. PMC+2PMC+2
5. Clinical Outcomes & Survivorship
Allograft MAT
- Systematic reviews and case series show significant improvement in pain and function (KOOS, IKDC, Lysholm) with 10–15-year graft survival rates ~70–85% depending on definition of failure and cartilage status. Orthopedic Reviews+2Dr. Brian J. Cole+2
- Age ≥40 is not an absolute contraindication; PRO improvement comparable to younger patients if cartilage is reasonably preserved. Dr. Brian J. Cole
Autograft (ST/PL)
- Rönnblad et al: pilot series of semitendinosus “neomeniscus” showed improvement in post-meniscectomy symptoms and function at mid-term, suggesting ST can act as a meniscal substitute. PMC
- Seitz et al: biomechanical study supports restoration of contact mechanics with ST lateral graft. PMC
- Case reports and small series (ST and PL for medial and lateral replacement) report good short-term pain relief and functional gains, but follow-up is usually ≤2 years. PubMed+4PMC+4PubMed+4
- A recent 2-year prospective comparative study (autograft vs allograft) reported better pain relief and quality of life with autografts (semitendinosus or patellar tendon) than with MAT, but with similar activity levels; authors emphasise need for longer follow-up. Esska Journals+2ResearchGate+2
So right now, MAT has stronger long-term evidence, while tendon autograft has promising short-term data but is still “under evaluation”.
6. Risks, Complications & Donor Site Morbidity
Meniscal Allograft
- Risks: graft extrusion, tearing, shrinkage, failure; re-operation and conversion to arthroplasty are not rare in high-risk cartilage. Orthopedic Reviews+2Dr. Brian J. Cole+2
- Theoretical risks of disease transmission and immune response, although modern tissue banking makes this very low. ScienceDirect
- No donor site morbidity.
Semitendinosus / Peroneus Longus Autograft
- Avoids immunologic and infectious risks of allograft and regulatory hassles of tissue banking. PMC+1
- Donor-site issues:
- ST harvest is familiar from ACL, usually minimal long-term deficit.
- PL harvest: ACL literature suggests good knee function without major ankle weakness, but careful selection is needed for high-demand ankle athletes. jccpractice.com+3Nature+3ijoro.org+3
- Long-term behaviour of the neomeniscus (degeneration, creep, extrusion) is unknown; all current enthusiasm is based on early results.
7. Availability, Regulation & Cost
- Allograft:
- Requires accredited tissue bank; in India this can be the rate-limiting step, with added costs and paperwork.
- Cost per graft is significant. ScienceDirect+1
- Autograft (ST/PL):
- Always available; no dependence on graft bank or import.
- Lower direct cost; theatre time and fixation implants are the major expense.
- Several authors specifically propose tendon autograft as a solution where MAT is “restricted by availability, legal issues and high cost.” Jisakos+4PMC+4PubMed+4
My Take (for your practice / website positioning)
If I had to summarise in one line for surgeons:
MAT remains the gold standard for biologic meniscal replacement because of its long-term data, but semitendinosus/peroneus-longus autograft “neomeniscus” is an exciting, lower-cost, immunologically safer alternative that is still in its evidence-building phase.
For India-type settings, your honest messaging could be:
- MAT where good tissue banking and funding exist, particularly in compliant, well-counselled young patients.
- Autograft reconstruction as a reasonable option in highly selected young, symptomatic post-meniscectomy knees where allograft is not accessible or cost-effective and preferably within a prospective study / registry.
Key References (you can drop into a paper / slide)
- Peters G, Smillie I. The current state of meniscal allograft transplantation and replacement. Knee. 2002. ScienceDirect
- Orthopedic Reviews – Meniscal allograft transplantation combined with ACL reconstruction: a systematic review. 2023. Orthopedic Reviews
- Frank RM et al. Do outcomes of meniscal allograft transplantation differ based on age and sex? 2022. Dr. Brian J. Cole
- Wei G et al. Comparison of medial versus lateral meniscus allograft transplantation. 2016. PMC
- Rönnblad E et al. Autologous semitendinosus tendon graft could function as a meniscal transplant after total or subtotal meniscectomy. KSSTA. 2022. PMC
- Seitz AM et al. Autologous semitendinosus meniscus graft significantly improves knee joint kinematics and contact mechanics. 2023. PMC
- Milenin O et al. Lateral meniscus replacement using peroneus longus autograft. Arthrosc Tech. 2020. PMC
- Kim Y et al. The potential of tendon autograft as meniscus substitution. JISAKOS. 2024. Jisakos
- Dong J et al. / Chi PC et al. Comparative review: allograft versus autologous tendon transplantation for meniscus reconstruction. 2024–25. Lippincott Journals+1

 Call us:+91-484 2885910 (Reception Orthopedics; 9am to 5pm Mon-Sat), +91-484-2885621 (22,23,24)
Doctor's mobile - +91 9497559755 (whatsApp anytime)
Call us:+91-484 2885910 (Reception Orthopedics; 9am to 5pm Mon-Sat), +91-484-2885621 (22,23,24)
Doctor's mobile - +91 9497559755 (whatsApp anytime)